Common Dental Myths
MYTH: There Is No Need In Seeing A Dentist If There Is No Visible Problem With My Teeth.
TRUTH: You must see your dentist twice a year, no matter what condition your teeth are in at the moment. If a problem has developed since your last visit, it can be resolved in the very early stages. Early de- tection and treatment of a problem is also more economical
MYTH: Not Brushing Causes Bad Breath
TRUTH: There are many other factors for bad breath( also know as halitosis). When the body ingests unpleasant smelling foods, such as garlic or onions, the odour remains until the body passes the food. Drinkers, smokers, dieters and sufferers of gastro- intestinal infections and sinusitis can also have chronic bad breath.
MYTH: Leave Wisdom Teeth In Until They Bother You
TRUTH: Once a wisdom tooth has become impacted, or misaligned, it can lead to problems such as an infection or periodontitis. A good rule to remember is to get them removed earlier as the procedure is easier and comes with less complications.
MYTH: Chewing Sugar-Free Gum After A Meal Is Just As Effective As Brushing
TRUTH: Although chewing gum can reduce plaque build-up and help to reduce acid levels in the mouth, it is not recommended in place of brushing and flossing to remove dental plaque and debris. Brushing and flossing are essential for removing bacteria building up on and in between teeth.
MYTH: Put Aspirin On An Aching Tooth
TRUTH: Only a good idea if the aspirin is taken orally. Placing it next to the tooth and gums can actually burn the gum tissue.
MYTH: Baby Teeth Are Not That Important
TRUTH: Baby teeth should be treated with the same care as adult teeth. If neglected, they can fall out sooner, resulting in crooked or malformed adult teeth.
MYTH: It’s Okay To Swallow Mouthwash
TRUTH: Mouthwashes are not meant to be ingested as they contain high levels of alcohol. The long terms affects of swallowing mouthwash can be dangerous and should be avoided.
MYTH: When The Gums Bleed, It Is Better Not To Brush The Teeth
TRUTH: Bleeding of gums is a sign that they are inflammed and are not healthy. This usually is a result of plaque and food particles accumulating around the teeth. Until this collection is removed, the gums continue to bleed. This is an indication that the individual needs to visit a dentist for treatment.
How a Dentist Can Detect an Eating Disorder
Dentists can be one of the first people to see the signs of an eating disorders in a patient.
Tooth erosion, sensitive teeth and bad breath are just a few of the signs that dentists use to identify whether a patient suffers from an eating disorder. These episodes bring stomach acids up through the mouth that are damaging to tooth enamel. Purging can damage the inside of the upper front teeth which weakens the tooth’s enamel causing sensitivity, thinning and chipping. Repeated exposure of these acids to the chewing surfaces of the lower teeth allows them to wear more easily and flatten or even concave causing further pooling.
Sometimes, eating disorders may not be discovered until too late, after irreversible damage has been done to the body as well as the teeth.
Although parents may not recognise that their children are anorexic or bulimic, they are often still taking the child to a dentist on a regular recall schedule.
Parents that suspect a child suffers from one of these disorders should consider visiting a dentist
An overview/snapshot of eating disorders today:
- Findings from a Victorian Adolescent cohort study revealed 8.8% of female adolescents had an eating disorder.
- 1 in 20 Australian women admitted to having suffered from an eating disorder while 1 in 4 individuals know someone who has an eating disorder.
- (http://www.eatingdisorders.org.au/ media/key-statistics.html)
Signs of an Eating Disorder:
- Bad breath
- Tender mouth, throat and salivary glands
- Eroded tooth enamel
- Teeth that are worn and appear almost translucent
- Mouth sores from excess vomiting
- Dry mouth
- Cracked lips
- Bleeding gums
- Sensitive teeth
Reducing stress can positively affect oral health
Earlier this year, the American Psychological Association concluded that over 80 percent of Americans rank money and the economy as significant causes of stress.
Chronic stress contributes to a number of health problems, including a weakened immune system and increased blood pressure, but it also takes its toll on periodontal health. If left untreated, periodontal disease may result in even more serious overall health complications.
Stress tends to make people more susceptible to harmful habits that negatively impact oral health, said Dr. David Cochran, president of the American Academy of Periodontology and chair of the Department of Periodontics at the University of Texas Health Science Centre at San Antonio.
“Stress may lead an individual to abuse tobacco or alcohol, and to possibly even neglect his or her oral hygiene,” said Dr. Cochran. “These lifestyle choices are known risk factors for the development of periodontal disease, which has been connected to several other chronic diseases, including heart disease and diabetes.”
In the February issue of the Journal of Periodontology, a study confirmed that stress interferes with oral hygiene. More than half of participants (56 percent) reported that stress led them to neglect regular brushing and flossing. Chronic stress is also associated with higher and more prolonged levels of the hormone cortisol, which can lead to a more destructive form of periodontal disease.
“During periods of high stress such as what we are currently experiencing in this economic climate, individuals should seek healthy sources of relief such as regular exercise, eating a balanced diet and getting adequate sleep,” said Dr. Cochran. “Doing so can help maintain a healthy mouth, and potentially help ward off other negative health concerns.”
Oral bacteria changes with obesity
Recent research published in the Journal of Dental Research suggest that oral bacteria may serve as a marker for the development of obesity.
The study’s researchers collected saliva from overweight women (those with a body mass index between 27 and 32). They identified and enumerated bacterial populations in the participants’ saliva samples by means of a DNA analysis, and they compared the levels with a control group.
Researchers found that seven species inves- tigated were present in measurably higher concentrations in the saliva of the over- weight women as compared to the control group. They also found that 98 percent of the overweight women could be identified by the presence of a single bacterial species at levels greater than one percent of the total salivary bacteria.
The results of the researchers’ analysis of these data suggest that the composition of salivary bacteria changes in overweight women. The investigators concluded that it seems likely that these bacterial spe- cies could serve as biological indicators of a developing overweight condition. Future research will investigate the role oral bacteria plays in the pathology but researchers believe in the possibility that oral bacteria may participate in the pathology that leads to obesity
Tongue stud ‘brain fatality risk’
Deadly brain abscesses should be added to the list of risks of having a tongue piercing, say doctors
In October, the BBC News reported how a 22-year-old man died in hospital following multiple brain abscesses weeks after getting his tongue pierced. His doctors warned that an infection in the bloodstream from the piercing reached his brain. More commonly, we see pain from swelling, prolonged bleeding, chipped or cracked teeth, gum recession and oral infections, though sometimes infections can reach the heart as well.
“The clear message is thatoral piercing is ill advised and should be avoided”
Professor Damien Walmsley Scientific adviser to the British Dental Association
Celebrities like Spice Girl Mel B and Princess Anne’s daughter Zara Phillips have had their tongues pierced.
But experts say people should think twice and put their health before fashion.
Problems associated with body piercing can be down to poor hygiene during the procedure or people failing to heed advice about follow-up care at home.
Look forward to your next clean with the Oraqix!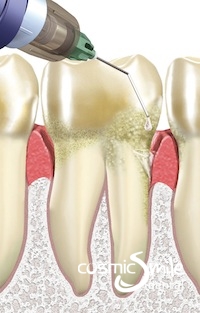
Probing and cleaning of the gums is vitally important in the diagnosis and maintenance of health. However, this can be a painful procedure for some people, meaning that an injection of local anaesthetic (LA) may be required. We know that this fear of injections means that sometimes appointments are cancelled or missed. This does not need to be a fear any longer as we now have the Oraqix non-injectable LA.
Made with lignocaine and prilocaine, it is placed into the pockets around teeth with a blunt ended applicator. And it works in 30 secs! In overseas studies, 69% of patients preferred the Oraqix LA compared to conventional injections even though the anaesthesia is not as deep. This makes sense as about a third of patients feel that the fear of the needle and its after-effects are the most distressing part of treatment.
The oraqix is easy to administer, safe and last for only 10-20 mins meaning that you won’t have that unpleasant numb feeling for hours afterwards. Best of all our sensitive patients that have had it so far love it and say that it makes their cleans a much more comfortable experience.

